Kidney Problems More Prevalent in NYC COVID-19 Patients
According To DBMI-Led Study Published In BMJ

Hospitalized COVID-19 patients at a New York City medical facility had higher rates of kidney complications than other COVID-19 patient groups in different areas of the U.S. and other countries, according to a new study from researchers at Columbia University Irving Medical Center and NewYork-Presbyterian.
The study, using data from electronic health records and published recently in the British Medical Journal, also found the need for mechanical ventilation was greatest at two different points after symptom onset.
The study offers a detailed look at the clinical course of the first 1,000 COVID-19 patients treated at NewYork-Presbyterian/Columbia University Irving Medical Center between March 1 and April 5, 2020.
Patients had higher rates of underlying conditions
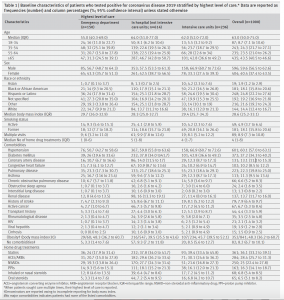
Patients in the study had higher rates of underlying chronic conditions than reported in other patient populations; the most common were hypertension (60%) and diabetes (37%). More than half of patients hospitalized for COVID-19 were male, and the median age was 63.
Nearly 34% of the patients admitted for COVID-19 developed acute kidney injury, versus 15% of patients in a recent report from China and 19% of patients in a report from Washington State. Almost 80% of patients in the ICU developed acute kidney injury.
Ventilators needed at two time points
The researchers also found that more than 95% of patients who were intubated required mechanical ventilation within the first 14 days, at either 3-4 days or 9 days after symptom onset.
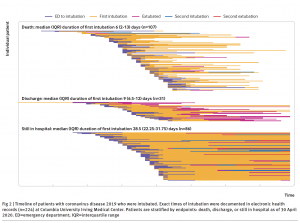
“The finding that there were two points in time to intubation for critically ill COVID-19 patients tells us when we might need to be most vigilant,” says George Hripcsak, MD, MS, chair and Vivian Beaumont Allen Professor of Biomedical Informatics at Columbia University Vagelos College of Physicians and Surgeons and co-corresponding author of the study. “Knowing that intubation is much less likely to be needed after 15 days can help clinicians decide if it is safe for a patient to return home.” Dr. Hripcsak is also director of medical informatics services for NewYork-Presbyterian/Columbia University Irving Medical Center.
Longer ICU stays
The median length of stay for COVID-19 patients in the current study was 6 days, similar to that of patients in a recent report from China. However, in the current study patients in the ICU had a median hospital stay of 23 days, compared with 8 days for critically ill patients in the Chinese study. More than a third of the critically ill patients remained hospitalized at the end of the study.
“Our study provides valuable details about the clinical course of hospitalized COVID-19 patients from one of the largest epicenters of the pandemic,” says RuiJun Chen, MD, a postdoctoral research fellow in biomedical informatics at Columbia University Irving Medical Center, clinical assistant professor of medicine at Weill Cornell Medicine, and co-corresponding author of the study. “As the pandemic continues to spread around the globe, our findings may have implications for planning and resource allocation to accommodate the needs of critically ill patients, and for de-escalation of care, rehabilitation, and follow-up care after prolonged stays on a ventilator or in the ICU.”
The overall mortality rate, around 21%, was similar to other patient cohorts. The mortality rate among ICU patients was 43.6%.
“Describing our COVID-19 patient population is the first step toward identifying important risk factors for experiencing severe disease,” says Hripcsak. “Additional studies are needed to tease out what is actually causing the differences we saw in our population versus other populations.”
Additional Information
The paper is titled “Characterization and clinical course of 1000 patients with coronavirus disease 2019 in New York: retrospective case series.”
Dr. Chen is also a hospitalist at NewYork-Presbyterian/Weill Cornell Medical Center.
Additional authors, all with Columbia University Irving Medical Center and NewYork-Presbyterian unless otherwise noted, are Michael Argenziano, Samuel Bruce, Cody Slater, Jonathan Tiao, Matthew Baldwin, Graham Barr, Bernard Chang, Katherine Chau, Justin Choi (Weill Cornell Medicine), Nicholas Gavin, Parag Goyal (Weill Cornell Medicine), Angela Mills, Ashmi Patel, Marie-Laure Romney, Monika Safford (Weill Cornell Medicine), Neil Schluger, Soumitra Sengupta, Magdalena Sobieszczyk, Jason Zucker, Paul Asadourian, Fletcher Bell, Rebekah Boyd, Matthew Cohen, MacAlistair Colquhoun, Lucy Colville, Joseph de Jonge, Lyle Dershowitz, Shirin Dey, Katherine Eiseman, Zachary Girvin, Daniella Goni, Amro Harb, Nicholas Herzik, Sarah Householder, Lara Karaaslan, Heather Lee, Evan Lieberman, Andrew Ling, Ree Lu, Arthur Shou, Alexander Sisti, Zachary Snow, Colin Sperring, Yuqing Xiong, Henry W Zhou, and Karthik Natarajan.
This study received no specific funding or grant from any agency in the public, commercial, or not-for-profit sectors. Individual support and other disclosures are included in the paper.
